|
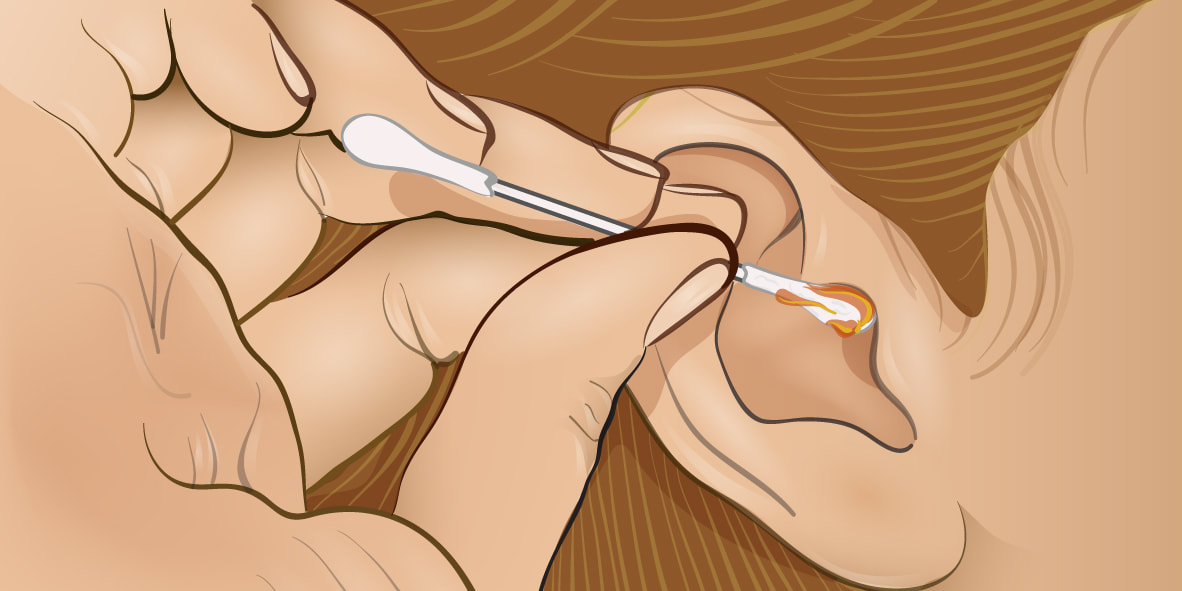
In the intricate landscape of healthcare, even the seemingly small matters can have significant impacts on overall well-being. Cerumen removal, commonly known as earwax removal, is one such aspect. Despite its universal presence, the approaches, tools, and perceptions surrounding cerumen removal vary globally. This article delves into the diverse practices and perspectives on global cerumen removal, highlighting its importance and the methods employed across different regions.
Understanding Cerumen: Cerumen, colloquially known as earwax, is a natural substance produced by the glands in the ear canal. Its primary function is to protect the ear by trapping dust, bacteria, and other foreign particles, preventing them from reaching the delicate eardrum. While cerumen usually clears itself through jaw movements, in some cases, it can accumulate and cause discomfort, impaired hearing, or even infection, necessitating removal. Global Perspectives on Cerumen Removal: The approach to cerumen removal varies significantly worldwide, influenced by cultural norms, medical practices, and available resources. In developed countries, such as the United States and parts of Europe, medical professionals often employ specialized tools like suction devices, curettes, or irrigation systems for cerumen removal. Procedures may take place in clinics or healthcare facilities, ensuring safety and efficacy under controlled conditions. Conversely, in resource-limited settings or rural areas, access to specialized equipment may be limited. Here, cerumen removal methods may be more rudimentary, relying on simple tools like ear drops, warm water irrigation, or manual extraction using cotton swabs or tweezers. While these methods may suffice for mild cases, they can carry risks of injury or infection if not performed carefully. Cultural Practices and Beliefs: Cultural beliefs also play a significant role in cerumen removal practices. In some cultures, cerumen is viewed as a symbol of cleanliness, and regular removal is considered essential for hygiene. Conversely, in others, there may be beliefs associating earwax with good health or spiritual significance, discouraging its removal unless necessary. These cultural perceptions influence individuals' attitudes towards cerumen removal and may impact their willingness to seek professional intervention. Challenges and Innovations: Despite advancements in medical technology, cerumen removal still poses challenges globally. Access to specialized care, particularly in remote or underserved areas, remains a concern. Additionally, improper cerumen removal practices, such as using cotton swabs, can lead to complications like impacted earwax or perforated eardrums. However, innovative solutions are emerging to address these challenges. Telemedicine platforms enable remote consultations, allowing healthcare providers to assess cerumen-related issues and provide guidance or referrals as needed. Furthermore, community-based initiatives, such as ear care education programs, raise awareness about safe cerumen removal practices, empowering individuals to take better care of their ear health. Cerumen removal is a universal aspect of healthcare that reflects the diversity of medical practices, cultural beliefs, and resource availability worldwide. While approaches may vary, the ultimate goal remains the same: to ensure ear health and well-being. By understanding and respecting these diverse perspectives, we can work towards universal access to safe and effective cerumen removal, promoting ear health for all, irrespective of geographical or cultural boundaries. Get more insights, On Global Cerumen Removal Explore More Related Topic on, Global Cerumen Removal
0 Comments
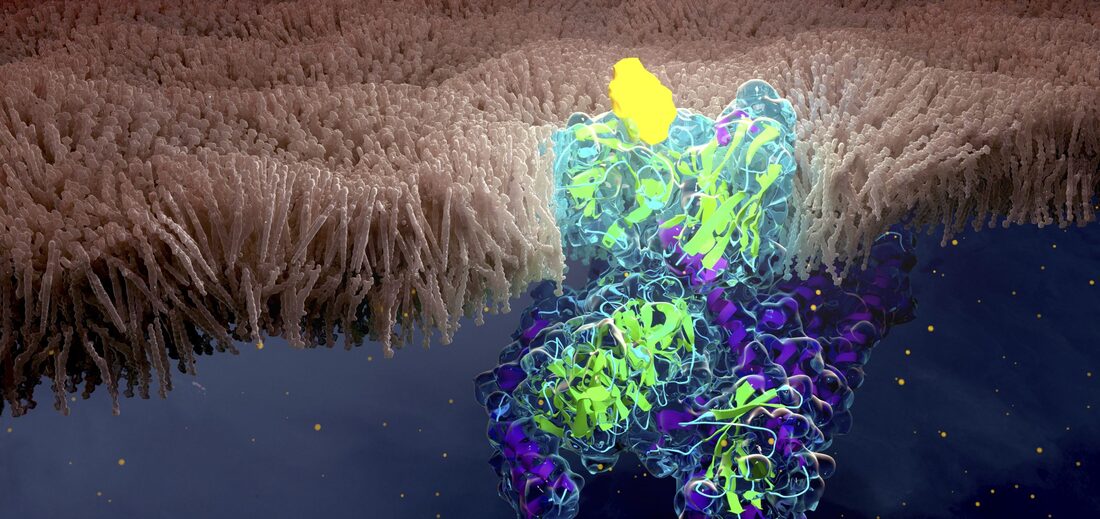
Global G-Protein Coupled Receptors (GPCRs) are a diverse and crucial class of proteins found in organisms across the globe, playing fundamental roles in various physiological processes. In this article, we delve into the intricacies of GPCRs, exploring their functions and significance in physiology. Understanding G-Protein Coupled Receptors: Global G-Protein Coupled Receptors also known as seven-transmembrane receptors, are cell surface receptors that transmit signals from the external environment to the interior of cells. They are involved in a wide range of biological processes, including sensory perception, neurotransmission, hormone regulation, and immune response. Structural Characteristics: GPCRs are characterized by their distinctive seven-transmembrane helical structure, which spans the cell membrane seven times. This structural arrangement forms a binding pocket on the extracellular side of the membrane, where ligands, such as hormones, neurotransmitters, or odorants, can bind and initiate signaling cascades within the cell. Functions of GPCRs: 1. Signal Transduction: GPCRs serve as molecular switches that relay signals from extracellular stimuli to intracellular signaling pathways. Upon ligand binding, GPCRs undergo conformational changes that activate heterotrimeric G proteins, leading to the activation of downstream effector molecules and cellular responses. 2. Sensory Perception: GPCRs play a crucial role in sensory perception, including vision, taste, olfaction, and touch. For example, rhodopsin, a GPCR found in rod cells of the retina, is essential for phototransduction and vision in low-light conditions. 3. Neurotransmission: GPCRs mediate neurotransmission by facilitating the release of neurotransmitters, such as dopamine, serotonin, and adrenaline, in response to synaptic input. These neurotransmitters bind to specific GPCRs on postsynaptic neurons, initiating signal transduction pathways that modulate neuronal excitability and synaptic transmission. 4. Hormone Regulation: Many hormones, including adrenaline, glucagon, and insulin, exert their effects through GPCRs. Hormone binding to GPCRs on target cells triggers intracellular signaling cascades that regulate cellular processes such as metabolism, growth, and gene expression. 5. Immune Response: GPCRs play a critical role in immune cell function and inflammation. Chemokine receptors, a subtype of GPCRs, regulate the migration and activation of immune cells in response to chemotactic signals, contributing to immune surveillance and host defense mechanisms. Significance in Physiology: The significance of GPCRs in physiology cannot be overstated, as they are involved in virtually every aspect of cellular communication and organismal function. Dysregulation of GPCR signaling has been implicated in numerous diseases and disorders, including cancer, cardiovascular disease, neurodegenerative disorders, and metabolic disorders. Global G-Protein Coupled Receptors (GPCRs) are essential molecular players in the complex landscape of cellular signaling and physiological regulation. From sensory perception and neurotransmission to hormone regulation and immune response, GPCRs orchestrate a myriad of biological processes that are vital for the health and functioning of organisms. Understanding the functions and significance of GPCRs not only sheds light on basic biological mechanisms but also holds promise for the development of novel therapeutic interventions for a wide range of diseases and disorders. Get more insights, On G-Protein Coupled Receptors Explore More Related Topic on, G-Protein Coupled Receptors Robotic process automation (RPA) uses artificial intelligence and machine learning to handle repetitive tasks, allowing healthcare providers to redeploy staff to more meaningful work that requires human skills and judgment. By automating routine administrative activities like data entry, background screening, registration and billing, RPA is helping to improve the accuracy and efficiency of clinical operations. Many providers are realizing productivity gains of 20-30% by using software robots to standardize workflows and reduce manual errors. This frees up clinicians and administrative personnel to focus on direct patient care.
Streamlining patient intake and billing Two areas ripe for automation are patient intake and insurance billing. Robotic Process Automation in Healthcare can extract and enter data from forms, applications and electronic health records much faster than humans. They eliminate clerical mistakes by precisely following standardized processes. For example, some hospitals use RPA bots to capture patient information at registration and populate billing systems in real-time. This accelerates check-in, reduces claims rejections and gets bills out the door more quickly. The automation of routine eligibility verifications and preauthorization requests with payers has also helped to shorten billing cycles and speed revenue collection. Accommodating rising administrative workload As the population ages and chronic diseases increase, healthcare organizations face growing administrative workloads just to keep pace with demand. Manual tasks now consume over 50% of clinical staff time according to some estimates. However, hiring and training support personnel is costly and staffing shortages are common across the sector. RPA counteracts these pressures by enabling a small number of software robots to work 24/7 performing repetitive chores without breaks or payroll overhead. This allows providers to meet compliance and reporting mandates that would otherwise stretch limited resources to the breaking point. Looking ahead, RPA will play an important role in managing administrative complexity as new policies and payment models evolve. Enhancing medical records management Electronic health records (EHR) have made patient information more accessible but also more difficult to manage at scale. Robotics is helping optimize clinical documentation and records digitization. For example, bots scan discrepancies in records, flag incomplete fields and ensure prescribed documentation standards are followed. They also autonomously retrieve, organize and upload files from disparate legacy systems into centralized EHR archives. This produces clean, standardized records that improve clinical decision making, regulatory compliance and reimbursement opportunities. Automated records management also aids care coordination across providers by keeping vital patient details up to date in real time. Improving supply chain logistics Healthcare supply chains face constant pressure to reduce costs while maintaining inventory readiness. Robotic process automation in healthcare simplifies replenishment, eliminates processing delays and prevents stock-outs through its 24/7 predictive monitoring of supplies, usage trends and automatic reordering. Robots track exact product locations, flag expiring items and orchestrate timely redistribution to outlying clinics and hospitals. Their inherent responsiveness helps lower overall inventory carrying costs compared to manual replenishment systems dependent on staff schedules. Automated logistics also enhances adherence to product recalls and safety alerts through lightning-fast notification workflows that protect patients and providers alike. Overall, robotic process automation in healthcare holds immense potential to transform healthcare administration by targeting tedious, repetitive manual tasks most vulnerable to human error. By deploying software robots to standardize high-volume workflows, providers realize productivity gains, data quality improvements and cost reductions that benefit both their bottom line and patient care. As clinical operations continue to complexify, RPA will play an increasing role stabilizing the infrastructure needed to deliver high quality, accessible and affordable healthcare. Its advantages of scalability, precision and 24/7 availability make it uniquely qualified to help the sector adapt to coming changes while prioritizing direct patient services above back-office functions. Get more insights, On Robotic Process Automation In Healthcare Explore More Related Topic on, Robotic Process Automation In Healthcare What are Transitional Care Management Services?
Transitional care management (TCM) services refer to the care and support provided to patients moving between different care settings, such as being discharged from a hospital to home or moving from a nursing home to home. The goal of transitional care is to ensure high-risk patients have the support and education needed to successfully transition and to prevent unnecessary readmissions or complications. Elements of Transitional Care Management Transitional Care Management Services typically involve several core components. Within two business days of discharge, the provider conducting TCM must communicate with the patient either face-to-face or via telehealth. During this initial communication, the provider assesses the patient's needs and medical issues to develop a core plan of care. This plan of care aims to address any health concerns or care gaps that could complicate the transition. It may involve scheduling follow-up appointments, managing medications, arranging for physical therapy or home healthcare, or ensuring the patient understands potential warning signs to watch out for. Ongoing Care and Coordination Following the initial visit, the transitional care provider remains actively involved in coordinating and managing the patient's care. This includes arranging referrals to specialists, consulting with other physicians on the patient's treatment plan, and communicating regularly with the patient to monitor symptoms and address new issues. The provider also coordinates with the facilities and health professionals involved in the patient's care both before and after discharge. Frequent communication ensures a smooth transition between settings and continuity of care. Transitional care management aims to bridge gaps that may otherwise lead to medical errors or preventable readmissions. Addressing Social Determinants of Health A comprehensive transitional care plan considers social factors like living situation, access to food/transportation, and caregiver support that could impact recovery and medication/treatment adherence. By addressing underlying social needs, transitional care aims to set patients up for success once medical oversight shifts from facilities to home-based care. This may involve referrals to community resources for food assistance, transportation vouchers, or home health aides. Transitional Care Management and Reducing Readmissions Research shows transitional care programs can significantly reduce preventable hospital readmissions, which are not only detrimental to patient health but also impose substantial costs on the healthcare system. Studies have found transitional care interventions lead to a 10-27% reduction in avoidable 30-day readmissions, especially among high-risk patients. By addressing care gaps, medication reconciliation issues, and social barriers to care, transitional care management helps patients stay on track with recommended treatments and follow-up care instead of relapsing soon after discharge. Proper transitional support sets up an environment where patients are empowered and able to successfully transition between settings without complications. Transitional Care Guidelines and Regulations To support transitional care delivery, Medicare developed provisions allowing billable TCM services following hospitalization. TCM codes were expanded in 2015 to include discharge from an inpatient hospital stay, partial hospitalization, skilled nursing facility, or community mental health center. Providers can bill for TCM by meeting with patients within two business days of discharge and providing at least 14 days of additional oversight like follow-up phone calls, medication adjustments and referrals for ongoing support. In 2021, transitional care codes generated over $900 million in Medicare reimbursements, reflecting growing recognition of the model's value. Many private insurers now also cover transitional care management services to improve patient outcomes. Transitional Care and the Future of Healthcare As the healthcare landscape evolves to reward quality over quantity, transitional care programs will further expand nationwide. Their ability to seamlessly coordinate complex care plans, reduce unnecessary utilization, and improve patient well-being makes TCM a win-win for all stakeholders. Healthcare organizations increasingly embed transitional support as a standard part of care delivery. As transitional care becomes integrated, patients will see fewer complications following medical events. With proper guidance, even high-risk patients can feel empowered managing at home. The future of effective transitional care lies in continued coordination between all partners, advanced digital connectivity, and addressing patients' full range of social and medical needs. As such models spread, the U.S. healthcare system moves closer to true seamless continuity of care. Get more insights, On Transitional Care Management Services Explore More Related Topic on, Transitional Care Management Services Congenital hyperinsulinism (CHI) is a rare genetic disorder characterized by excessive insulin production in the pancreas, leading to low blood sugar (hypoglycemia). This condition can have serious health implications, particularly for infants and young children. In this article, we'll explore the causes, symptoms, and treatment options for congenital hyperinsulinism.
What Is Congenital Hyperinsulinism? Congenital Hyperinsulinism Treatment is a disorder that affects the way the pancreas regulates insulin production. In CHI, the pancreas produces too much insulin, which can cause blood sugar levels to drop dangerously low. This can lead to a range of symptoms and complications if not managed properly. Causes of Congenital Hyperinsulinism CHI is caused by genetic mutations that affect the function of the insulin-producing cells in the pancreas. These mutations can be inherited in different ways, including autosomal recessive and autosomal dominant inheritance patterns. The condition may also be associated with other genetic syndromes. Symptoms of Congenital Hyperinsulinism Common symptoms of CHI include:
1. Medical Management: · Frequent feedings: To maintain stable blood sugar levels, frequent feedings (including nighttime feedings) may be necessary. · Medications: Drugs such as diazoxide and octreotide can help regulate insulin production and blood sugar levels. 2. Surgical Interventions: · Pancreatectomy: In severe cases, partial or near-total removal of the pancreas may be necessary to control insulin production. 3. Monitoring and Follow-Up: · Blood sugar monitoring: Regular monitoring of blood sugar levels is crucial to manage the condition and prevent complications. · Long-term follow-up: Ongoing follow-up with a pediatric endocrinologist is important for managing the condition and monitoring development. Congenital hyperinsulinism is a challenging condition that requires careful management to prevent complications and support healthy development. Early diagnosis and treatment are key to managing CHI effectively. If you suspect your child may have CHI, consult a healthcare professional for proper evaluation and treatment. Get more insights, On Congenital Hyperinsulinism Treatment Explore More Related Topic on, Congenital Hyperinsulinism Treatment West Nile Virus (WNV) poses a significant public health concern, particularly during the warmer months when mosquito activity is at its peak. As a mosquito-borne illness, WNV can cause serious neurological complications in humans, making it essential for individuals to be informed about the risks, symptoms, and prevention strategies associated with this viral infection. In this article, we delve into the intricacies of West Nile Virus and discuss effective branding strategies for raising awareness and promoting prevention efforts.
1. The Threat of West Nile Virus West Nile Virus is a flavivirus commonly transmitted to humans through the bite of infected mosquitoes, primarily of the Culex species. While many individuals infected with WNV may remain asymptomatic, others may develop mild to severe symptoms, including fever, headache, body aches, joint pain, vomiting, diarrhea, and in rare cases, neurological complications such as encephalitis or meningitis. Key Facts About West Nile Virus:
2. Raising Awareness and Promoting Prevention Effective branding plays a crucial role in raising awareness about West Nile Virus and promoting preventive measures to reduce the risk of infection. By conveying clear, concise messaging and emphasizing the importance of personal protection and mosquito control, branding efforts can empower individuals and communities to take proactive steps to prevent the spread of WNV. Branding Strategies for West Nile Virus Awareness:
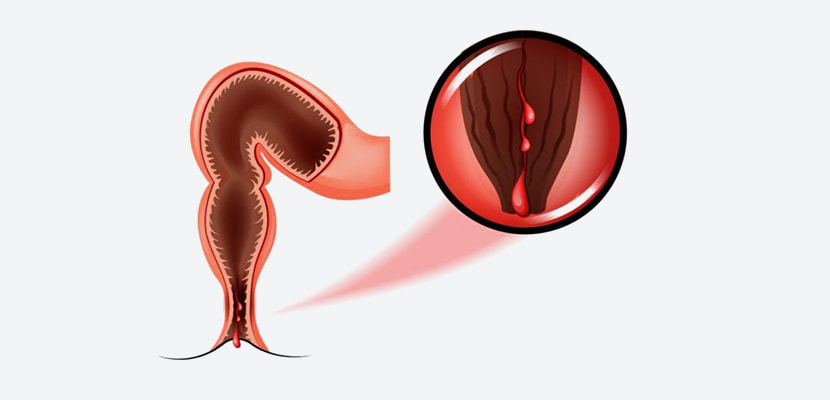
Get more insights, On West Nile Virus Top of Form Explore More Related Topic on, West Nile Virus Introduction: While conventional medical treatments play a crucial role in managing anal fissures, some individuals may seek natural remedies as complementary or alternative options. This article aims to explore various holistic approaches to anal fissure treatment, focusing on natural remedies that may offer relief from symptoms and promote healing.
Herbal Remedies and Supplements: Certain herbs and supplements are believed to have anti-inflammatory, soothing, and healing properties that may benefit individuals with anal Anal Fissure Treatment Discussing the potential benefits of ingredients like aloe vera, witch hazel, and psyllium husk can provide readers with insight into how these natural remedies may help alleviate discomfort and promote tissue repair. Lifestyle Modifications and Self-Care Practices: In addition to herbal remedies, lifestyle modifications and self-care practices can play a significant role in managing anal fissures naturally. This section can explore techniques such as sitz baths, proper hygiene practices, and stress reduction strategies, emphasizing their role in reducing symptoms and supporting overall anal health. While natural remedies may not replace conventional medical treatments for anal fissures, they can serve as valuable adjuncts to promote healing and alleviate symptoms. By incorporating herbal remedies, supplements, and lifestyle modifications into their treatment plan, individuals can take a holistic approach to managing anal fissures and improve their quality of life. As always, it's essential to consult with a healthcare professional before starting any new treatment regimen. Get More Insights, On Anal Fissure TreatmentTop of Form Per-Encounter Medical billing is a billing model widely used in healthcare settings to bill patients or their insurance providers for individual services rendered during a single encounter or visit. This billing model plays a crucial role in revenue generation for healthcare providers and helps ensure fair compensation for the services provided. Here's a closer look at the role of per-encounter billing in healthcare and its impact on providers and patients.
Key Features of Per-Encounter Medical Billing 1. Itemized Billing: Per-encounter billing itemizes each service provided during a healthcare encounter, such as consultations, diagnostic tests, treatments, and procedures. Each service is assigned a specific code that corresponds to a predetermined fee, allowing for accurate tracking of revenue and expenses. 2. Fee-for-Service Model: Per-encounter billing operates on a fee-for-service model, where patients or their insurance providers are billed based on the actual services rendered during the encounter. This model contrasts with other billing models, such as capitation or bundled payments, which may involve flat fees or monthly premiums regardless of the services provided. 3. Flexibility for Providers: Per-encounter billing provides flexibility for healthcare providers to bill for services based on their actual time and resources expended during each encounter. Providers can adjust their billing practices based on the complexity of the services provided, the patient's medical condition, and other relevant factors. Impact on Healthcare Providers 1. Revenue Generation: Per-encounter billing is a primary source of revenue for healthcare providers, particularly in fee-for-service environments such as private practices and outpatient clinics. By accurately billing for each service provided, providers can generate revenue to cover operational expenses and invest in quality improvement initiatives. 2. Resource Allocation: Per-encounter billing allows healthcare providers to track their revenue and expenses more effectively, enabling them to allocate resources efficiently and identify areas for improvement. Providers can use billing data to assess the profitability of different services, evaluate the cost-effectiveness of treatments, and optimize their practice operations. Impact on Patients 1. Transparency: Per-encounter billing provides transparency to patients regarding the cost of each service provided during their healthcare encounter. Patients receive itemized bills that clearly outline the services rendered and their associated costs, allowing them to understand their healthcare expenses and make informed decisions about their care. 2. Insurance Reimbursement: Patients with health insurance may have their per-encounter medical bills covered partially or fully by their insurance provider, depending on their plan coverage and benefits. Patients should review their insurance policy to understand their coverage and any out-of-pocket expenses they may incur. Per-Encounter Medical billing is a fundamental component of healthcare finance that plays a critical role in revenue generation for providers and transparency for patients. By accurately billing for each service provided during a healthcare encounter, providers can generate revenue to support their practice operations and investments in quality improvement. Patients benefit from transparency regarding their healthcare expenses and insurance coverage, allowing them to make informed decisions about their care. As healthcare continues to evolve, per-encounter billing will remain an essential tool for providers and patients alike in navigating the complexities of the healthcare system. Get More Insights, On Per-Encounter Medica Nicotine Replacement Therapy (NRT) is a proven method for helping individuals quit smoking by providing a controlled dose of nicotine to alleviate withdrawal symptoms and cravings. When used correctly and in combination with counseling and support, NRT can significantly increase the chances of successful smoking cessation. Here are some tips for using NRT effectively to quit smoking:
1. Consult with a Healthcare Provider: Before starting Global Nicotine Replacement Therapy it's essential to consult with a healthcare provider to discuss your smoking habits, medical history, and suitability for NRT. Your healthcare provider can help you choose the most appropriate form of NRT and develop a personalized quitting plan. 2. Set a Quit Date: Choose a specific quit date and commit to quitting smoking entirely on that day. Setting a quit date gives you a clear goal to work towards and helps mentally prepare you for the challenges of quitting. 3. Use NRT as Directed: Follow the instructions provided with your chosen form of NRT carefully. Whether you're using nicotine patches, gum, lozenges, inhalers, or nasal sprays, it's essential to use them as directed to maximize their effectiveness in managing cravings and withdrawal symptoms. 4. Start with the Right Dosage: Begin NRT with the appropriate dosage based on your level of nicotine dependence and smoking habits. Nicotine patches come in different strengths, while gum, lozenges, inhalers, and nasal sprays offer various options for dosage and frequency of use. Starting with the right dosage ensures adequate relief from cravings without overstimulating nicotine receptors. 5. Combine NRT with Behavioral Support: While NRT can help alleviate physical cravings, addressing the behavioral and psychological aspects of smoking is also crucial for successful quitting. Consider combining NRT with behavioral support, such as counseling, support groups, or self-help resources, to develop coping strategies and overcome triggers for smoking. 6. Gradually Taper Down NRT: As you progress in your quit journey, gradually taper down your use of NRT to reduce nicotine dependence. Many NRT products offer step-down options with lower nicotine concentrations or fewer doses per day, allowing you to wean yourself off nicotine gradually while minimizing withdrawal symptoms. 7. Stay Persistent and Patient: Quitting smoking is a challenging process that requires persistence and patience. It's normal to experience setbacks and cravings along the way, but don't get discouraged. Stay committed to your quit journey, celebrate small victories, and seek support from friends, family, or healthcare professionals when needed. 8. Monitor Your Progress: Keep track of your progress and celebrate milestones along the way. Whether it's one day, one week, or one month smoke-free, each achievement is a step towards better health and well-being. Use tools like quit journals or mobile apps to record your progress and stay motivated. Nicotine Replacement Therapy (NRT) is a valuable tool for individuals looking to quit smoking. By following these tips and incorporating NRT into a comprehensive quitting plan, you can effectively manage cravings and withdrawal symptoms, increase your chances of long-term success, and embark on a journey towards a smoke-free life. Remember, quitting smoking is a journey, and with determination, support, and the right resources, you can achieve your goal of becoming smoke-free. Get More Insights, On Nicotine Replacement Therapy When it comes to staying healthy, our immune system plays a critical role in defending against pathogens and keeping us feeling our best. While there’s no magic pill for immunity, certain natural remedies can give your body an extra edge in fighting off illness. Here are ten potent immune boosters to incorporate into your wellness routine:
Elderberry: Rich in antioxidants and vitamins, elderberry syrup has been shown to reduce the duration and severity of cold and flu symptoms. Garlic: This pungent bulb contains allicin, Natural Immune Booster a compound with antimicrobial properties that can help ward off infections and support immune function. Ginger: Known for its anti-inflammatory and antibacterial properties, ginger can help strengthen the immune system and alleviate symptoms of respiratory infections. Turmeric: Curcumin, the active compound in turmeric, boasts powerful antioxidant and anti-inflammatory effects, making it a valuable ally in immune health. Citrus Fruits: Packed with vitamin C, citrus fruits like oranges, lemons, and grapefruits help stimulate the production of white blood cells, key players in immune defense. Probiotics: These beneficial bacteria promote a healthy gut microbiome, which is essential for proper immune function. Yogurt, kefir, and fermented foods are excellent sources of probiotics. Green Tea: Loaded with antioxidants called catechins, green tea can enhance immune function and may offer protection against viral infections. Honey: Raw honey is not only delicious but also contains antimicrobial properties that can help soothe sore throats and boost overall immunity. Mushrooms: Varieties like shiitake, reishi, and maitake are rich in beta-glucans, compounds that enhance immune function and may help fight infections. Dark Leafy Greens: Spinach, kale, and Swiss chard are packed with vitamins A, C, and E, as well as antioxidants that support immune health. Incorporating these natural immune boosters into your diet and lifestyle can help strengthen your body’s defenses and reduce your susceptibility to illness. However, it’s essential to remember that maintaining a balanced diet, getting regular exercise, managing stress, and prioritizing sleep are all crucial components of a healthy immune system. By combining these strategies, you can bolster your immunity and enjoy greater vitality and wellbeing year-round. Get More Insights, On Natural Immune Booste |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |





 RSS Feed
RSS Feed
